Clinical depression, also known as major depressive disorder, is one of the most common mental health conditions. An estimated seven percent of adults in the U.S. experience its effects each year. Adults with clinical depression encounter symptoms such as loss of interest in activities, trouble concentrating, remembering things, feelings of sadness, guilt, emptiness, irritation, hopelessness, or worthlessness. Many people don’t realize is that it comes with many physical symptoms as well, including headaches, digestive problems, changes in appetite, and sleep issues. These symptoms tend to be so severe that they drastically affect people’s lives and make it difficult for them to complete simple, day-to-day tasks.
Because clinical depression is so rampant, most people know at least one person who has dealt with this condition, even if they haven’t experienced it themselves. It can be easy to take the wrong approach when trying to help a friend, coworker, or family member with clinical depression, so it’s essential to take a step back and assess your plan to make sure that you don’t do more harm than good.
Don’t trivialize their feelings or take a “tough love” approach.
Many people who know someone with clinical depression try to help by offering words of encouragement, but that – although usually well-intentioned – can make things even worse. Saying things like “it’s all in your head” or “just cheer up” can do more harm than good, especially when someone is already dealing with feelings of guilt or worthlessness. It’s important to remember that clinical depression, like other mental disorders, is a valid illness. The brain is an organ, and it can get sick and malfunction just like any other organ.
Similarly, it’s vital to avoid steering the conversation back to focus on you. Sometimes, when someone tries to help a loved one, they attempt to console them by sharing personal stories and trying to relate to them. The idea behind this is, of course, to make the struggling person feel like they’re less alone. It’s effortless to start a sentence with, “When I feel depressed…” However, to a person with clinical depression or in the throes of another mental illness, such language can make it seem like you’re invalidating their feelings. It’s important to remember that having clinical depression is different from “feeling depressed.” Everyone experiences feelings of sadness at times, but people with clinical depression experience these negative feelings almost regularly, for an extended time, and sometimes seemingly without probable cause.
Do listen and validate.
Let your friend talk about their feelings (if they want to), and respond with words of validation rather than simple encouragement. Experiencing the intense emotional symptoms caused by clinical depression can make a person feel out of control and like there’s something fundamentally wrong with them. The feelings of isolation and worthlessness that follow tend to compound upon themselves. You may find that your friend starts blaming themselves for their beliefs and questions why they don’t necessarily line up with reality. “I have a job I enjoy, a partner I love, and a beautiful house. So, why am I so unhappy?”
Help your friend put the situation into perspective. When a person with clinical depression spirals down into hopelessness, you are in a unique position to speak as a third party who’s partially removed from the situation. This can be highly beneficial for a person with any variety of mental illness, which is why talk therapy is often so effective.
Just because someone’s feelings don’t accurately reflect reality doesn’t make them invalid or unimportant. While it’s important to recognize when emotions, thoughts, and reality don’t line up (which is a useful aid in combating mental illness), it can also be empowering for people to be assured that the validity of their feelings is not dictated by how closely they resemble reality. That their feelings exist is enough to make them valid.
Don’t judge (but don’t avoid either).
The last thing you want to do is make your loved one feel judged. They’re probably already judging themselves enough as it as, after all. Don’t point out all of the responsibilities that they’re neglecting while they try to stay afloat; they most likely already know, and that knowledge is probably making their symptoms worse. (Depression is the epitome of a vicious cycle.) Keep in mind, however, that in your effort to refrain from judging, you may be overcompensating, which can have a similar effect to upfront judgment if it’s apparent that you’re going out of your way to avoid mentioning the issue.
Do confront with compassion.
Make yourself available, and make sure your friend knows that you’re there for them. It is challenging for someone to pull themselves out of a depressive episode on their own, and for some people, it’s impossible. Ask your friend what you can do to help. You could suggest things like walking their dog or doing their laundry, but it’s often better to ask them what they need because it ensures that you don’t come off sounding accusatory. Remember that clinical depression – especially when combined, as it often is, with another disorder like anxiety – tends to make people blow up minor problems into catastrophes. For this reason, it’s better to tread carefully and approach things delicately.
Alternatively, you could cook them a meal and bring it to their house. This gesture, though simple, is an ideal way to show your friend that you care. After all, one of the primary physical symptoms of clinical depression is a loss of appetite. Some people claim that they’re so busy worrying that they forget to eat.
Don’t smother them with your presence or force them to participate in social activities.
You may be inclined to make yourself so available to your friend that you start to overwhelm them. While your intentions are undoubtedly honorable, being around people with whom they feel they cannot correctly make people with clinical depression feel even more isolated than if they were alone.
If they do decide to accept your offers to spend time with them, be careful not to take them out for a night on the town or to a party where alcohol is readily available. Alcohol affects neurotransmitters like serotonin, which are thought to play a role in many mental health conditions. For this reason, people with clinical depression are more likely to experience the harmful effects of alcohol, and alcohol can exacerbate their depression symptoms. Also, people with clinical depression are more likely to develop problems with alcohol abuse, and most antidepressant medications should not be mixed with alcohol.
Do let them know that you’re there for them.
Make a point to regularly text them, letting them know that you are available for anything they might need (or want). Invite them to participate in social activities with you, especially relaxing ones with a few close friends, low stakes, and no alcohol. Make sure they know that you still value their friendship and want to spend time with them, but let them know that it’s not mandatory, and don’t be offended when they’re not in the mood.
It’s essential to keep the lines of communication open, but you don’t want your friend to feel like they don’t have the agency to make their own decisions. They need to know that, sometimes, it’s okay to give in and not get out of bed for a day. There’s always tomorrow.
Don’t prescribe a one-size-fits-all solution.
If you’ve struggled with clinical depression yourself or know other people who have, you may be tempted to share what worked for you. While it can be helpful to try to relate to your struggling loved one and offered them some hope, it can also make them feel inadequate or, even worse, irreparably broken. Likely, the person has already tried many of the solutions you offer, and it can be exhausting to hear the same suggestions over and over again. It’s also important to remember that what works for one person might not work for the next.
Do help them research treatment options.
After making sure that the person knows that they’re under no obligation to accept help from you, gently offer to help them find options to treat their clinical depression. For example, perhaps your friend was recently diagnosed and hasn’t tried many of the options out there, or maybe they feel like they’ve tried everything and nothing has worked. There are many ways to treat clinical depression, including medications (like SSRIs, which affect brain chemistry), various types of talk therapy, and lifestyle changes like implementing an exercise routine. However, around 40 percent of people with clinical depression find that traditional medications and treatments don’t give them as much relief as they hoped.
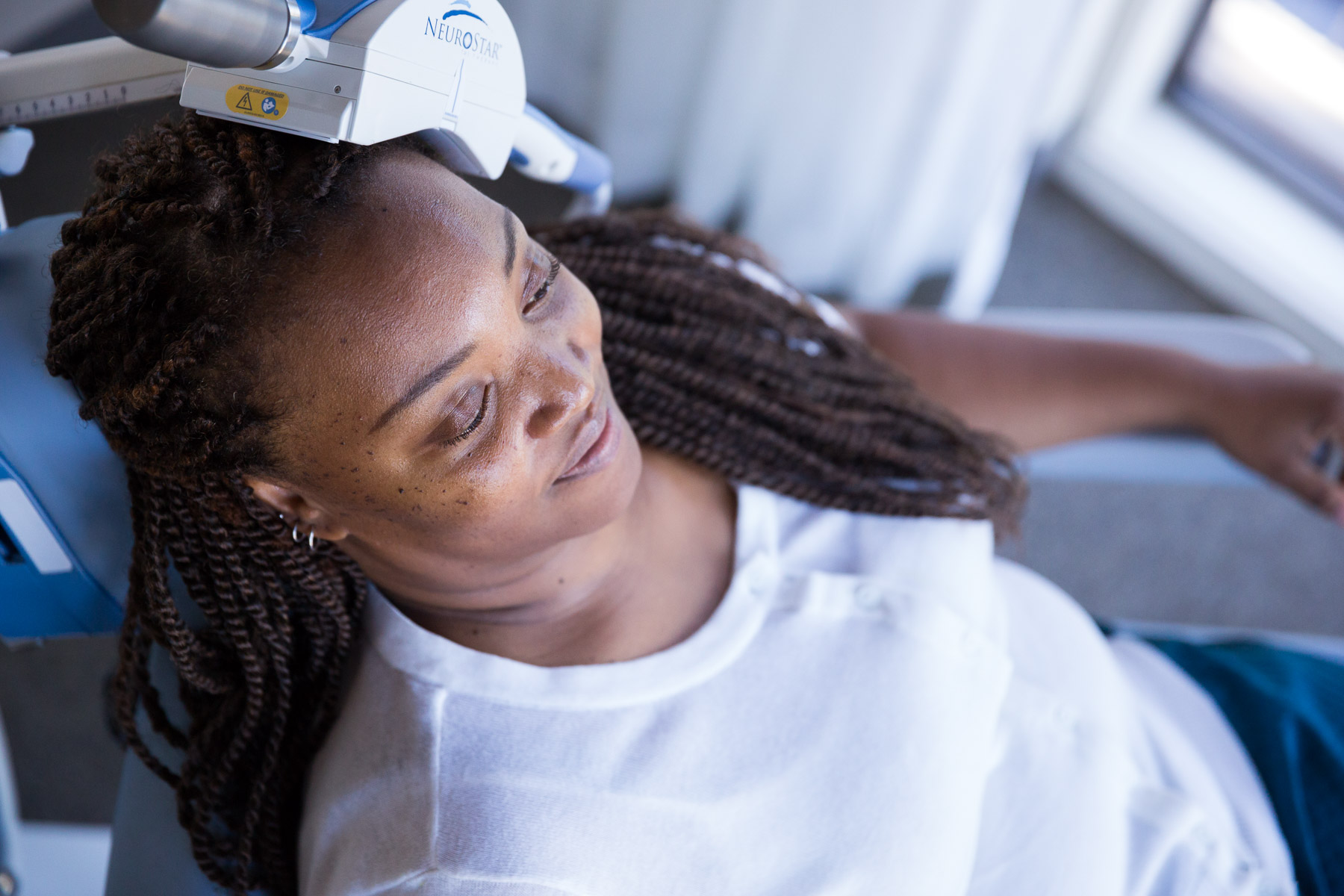
The good news is that there is hope for people with treatment-resistant depression. An innovative therapy called transcranial magnetic stimulation, also known as TMS therapy, is an option that’s often used in conjunction with medication, talk therapy, and lifestyle changes to help those who haven’t found relief. First, a practitioner places a metal coil on the client’s forehead. This coil then transmits magnetic pulses into the brain, specifically targeting the bilateral prefrontal cortex, thereby stimulating the nerve cells in the part of the brain that regulates mood. The procedure is noninvasive and requires no hospitalization or anesthesia. Many people don’t experience any side effects, but when they occur, they tend to be mild and short-lived.
Because TMS therapy requires multiple treatments, each of which lasts between 30 and 60 minutes, it’s essential to find a reliable provider. Mindful Health Solutions has 12 locations, eleven in Northern California and one in Southern California, and with another opening in October in Fairfield. Each of these locations relies on a team of providers who strive to treat disorders like treatment-resistant clinical depression with a compassionate and patient-centered approach.