What Is Ketamine Therapy? Discover This Revolutionary Therapy That’s Changing the Landscape of Major Depression Treatment.
Not finding relief from existing depression treatments like medications, TMS, or therapy? Ketamine Infusion Therapy (KIT) may be a potential treatment option to help restore your quality of life. KIT is effective for patients struggling with a number of psychiatric conditions, including Treatment-Resistant Depression (TRD), Major Depressive Disorder (MDD), anxiety disorders, Post-Traumatic Stress Disorder (PTSD), Obsessive-Compulsive Disorder (OCD), and suicidal ideation.
Mindful Health Solutions is here to guide you on the path to lasting depression relief. Our clinicians specialize in IV ketamine therapy for depression, with plans customized to your specific needs.
Trusted Experts in IV Ketamine Therapy
Mindful Health Solutions is a leading provider of cutting-edge interventional psychiatry treatments, including Ketamine Infusion Therapy for treatment-resistant depression. Led by Chief Medical Officer Dr. Toby Marton and Associate Chief of Training and Innovation Dr. Alvin Lau, our team has extensive experience and expertise in ketamine infusion treatment plans, transforming hundreds of lives and publishing vital research in top medical journals.
We provide IV ketamine infusion treatments in a relaxed outpatient setting, ensuring safety and minimal side effects. Our goal is to help you find relief from the debilitating symptoms of depression, rediscover joy, and improve your quality of life. Trust us for safe, effective ketamine therapy on your journey to mental wellness.
Antidepressants Aren’t Always the Answer

1 in 3
people struggling with depression have Treatment-Resistant Depression (TRD), meaning they don’t respond to medications.

Recovery
with with Ketamine Infusion Therapy is 2.5x more likely for patients who failed 2+ medications
What does ketamine infusion therapy treat?
People who are currently struggling with Major Depressive Disorder (MDD) and haven’t found success or have experienced adverse side effects from at least two different antidepressant treatments may have Treatment-Resistant Depression (TRD). Clinical studies show that ketamine infusion therapy can effectively treat MDD and TRD with a success rate as high as 49%. Many patients show rapid improvement after just their first or second IV ketamine infusion.
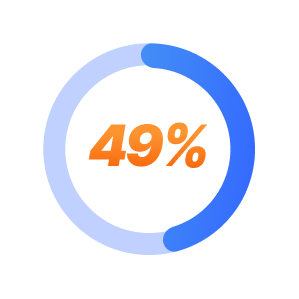
49% of patients show improvement in depression symptoms after ketamine infusion therapy.
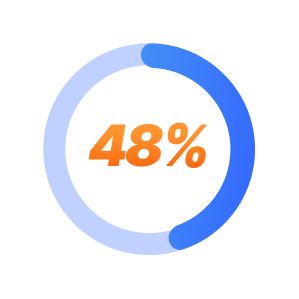
48% of patients show improvement in anxiety symptoms after ketamine infusion therapy.

6 induction sessions across 6 weeks
McInnes et al. 2022 and Hietamies et al. 2023
Why Mindful Health Solutions for Ketamine IV Therapy?
Ketamine therapy is a novel depression treatment; not all clinics can provide the same expert and safe medical care as we can at Mindful Health Solutions. Our IV ketamine treatment clinics are run by expert mental health clinicians in the field; they have years of expertise using ketamine infusion therapy to treat mental illness and have conducted and published peer-reviewed research on ketamine in top medical journals. You can trust that they will only recommend ketamine infusion therapy as a treatment option if it is safe and they believe it will help you finally experience the relief from mental illness that you deserve.
At Mindful Health Solutions, we understand the importance of patient-centered care and understand that one size does not fit all when it comes to mental health treatment. This is why we pride ourselves on offering cutting-edge alternative interventional therapies such as TMS, Intranasal Esketamine (Spravato), and ketamine infusion therapy, alongside standard treatment options such as medications and psychotherapy.
Mindful Health Solutions also wants to make depression therapy comfortable and accessible. If patients are unable to physically come into the office for consultation or prefer a virtual appointment, Mindful Health Solutions offers telepsychiatry. We also foster a strong culture of Diversity, Equity, and Inclusion. Our mental health care clinicians and therapists strive to embody a sense of awareness, respect, and humility with regard to cultural differences. And last but not least, we accept most major insurances.
Frequently Asked Questions
How much does ketamine therapy cost?
Wondering, what does ketamine therapy cost and is it covered by insurance? We're here to help answer your questions prior to treatment.
IV ketamine therapy for depression, including major depression, or other psychiatric indications is $450 per session for induction treatments (first 6 sessions) and $400 per session for maintenance treatments. The number of IV ketamine for depression treatments may vary per patient, with most patients completing between 6-12 IV ketamine treatments.
With the exception of Kaiser, VA, and TriCare/TriWest insurance, ketamine infusion therapy is not eligible for insurance at this time. However, IV ketamine treatment may be eligible for some reimbursement with a Flexible Spending Account (FSA) or Health Savings Account (HSA). Coverage will vary depending on the specific FSA or HSA plan and your health insurance carrier. Therefore, we recommend that you contact your insurance plan before treatment.
Note that pricing remains the same across all locations in Sacramento, Oakland, San Francisco, and Austin clinics. Payment plans are available at each clinic.
How do you feel during treatment?
Ketamine infusion treatments are often described as an “out-of-body experience.” Patients may experience dissociation, often reported as a pleasant feeling that relieves symptoms of depression. Dissociation can include:
- Feeling detached from your body
- Having a distorted perception of time and space
- Experiencing altered perceptions and sensations
- Entering a dream-like state where thoughts may become distorted
- Emotional detachment
Some individuals describe a sense of mental clarity or expanded consciousness during IV ketamine for depression.
How effective is IV ketamine therapy?
Wondering, how does ketamine therapy work?
Clinical studies show that ketamine infusion therapy can effectively treat Major Depressive Disorder and Treatment-Resistant Depression with a success rate as high as 70%. Many patients show rapid improvement after just their first or second IV ketamine treatment infusion.
How are ketamine infusions administered?
You may be asking yourself, how does ketamine work?
Ketamine Infusion Therapy treatments are administered in one of our certified treatment clinics. The session will begin by getting the patient situated in a comfortable chair and your clinician will get you settled with the IV. Your clinician will inform you when the IV has started. The infusion lasts 40 minutes and the entire session takes about 90 minutes to complete.
What does a ketamine therapy session look like?
IV ketamine therapy is an office-based, outpatient procedure. The ketamine infusion lasts 40 minutes and the entire session takes about 90 minutes to complete. The session process will begin by getting you situated in a comfortable chair. Then, your clinician will inform you when the IV has started.
The first thing you will feel is a sense of relaxation of mind and/or body. You may then begin to feel slightly light or light-headed. Some people report a sense of feeling a slight warmth. Eventually, you may feel even lighter, almost a slight separation between yourself and your body. Your hands and legs may feel far away. Some people progressively feel more separation between themselves and the different components of consciousness (e.g., their thoughts, feelings, bodily sensations, and perception). Occasionally, people continue to progressively experience an even greater physical sensation of lightness – sometimes to the point of feeling above the room. Patients generally tolerate these sensations very well, reporting the experience as “spiritual” or “pleasurable.”
If someone is struggling with depression, anxiety, or rumination, this point is when they feel much less of and/or distant from these feelings. This experience is frequently described as an immense relief – like the blanket of depression has been temporarily lifted. This experience can also serve as a very hopeful reminder to patients that depression or anxiety does not define them. These conditions are separate from them, and as such, they can be temporary.
In rare cases, patients may have a more negative experience after receiving a ketamine intravenous injection. We have psychiatric professionals on-site to help manage these rare events, which are generally brief and usually resolve completely within 10-15 minutes after stopping the infusion.
Reach out today to learn more about the process during ketamine infusion treatments.
Are there any side effects of ketamine infusion therapy?
The most common ketamine therapy side effects usually only occur up to two hours after the ketamine infusion has been administered. To help ensure the safety of patients, there is a two-hour window of supervision at the clinic following the administration before patients can leave and head home.
Although you may not experience any of these IV ketamine side effects, the most common include:
- Double vision
- Loss of appetite
- Dream-like state
- Nausea
- Elevated blood pressure
- Trouble speaking
- Slight pain at the injection site
- Dissociation or feeling strange/loopy
How many sessions should I expect?
Initial ketamine infusion therapy consists of 6 IV ketamine treatments over the course of 3 weeks. The details of this protocol are discussed in detail during the initial evaluation. Infusion appointments generally take 90–120 minutes. If the symptoms are successfully controlled with these initial treatments, then follow-up evaluations will be conducted to determine long-term treatment plans.
Maintenance treatments for IV ketamine for depression usually consist of one infusion every 2-4 weeks.
